- By Marketing
- In Mold Removal
Lyme Disease and the Many Symptoms It Can Present in Humans

When it comes to Lyme disease, there is a number of important factors that all must be addressed for proper diagnosis and treatment of the disease. The complications that arise from the many opportunistic co-infections that are traditionally present in Chronic Lyme disease sufferers makes diagnosis based on the most common laboratory findings very inaccurate. However, recognizing which symptoms an individual may be experiencing is the first step towards recognizing Lyme disease as a possible diagnosis and seeking effective treatment.
Chronic Lyme disease is one of the most difficult diseases to treat, partially due to the lack of effective diagnostic methods, and because of its ability to mimic other diseases. Lyme disease is known as the “great imitator” because its symptoms resemble over 300+ different and more well-known diseases. Some of these symptoms include fatigue, joint pain, poor sleep, muscle skeletal pain, muscle stiffness, mood problems, depression, anxiety, loss of concentration, short term memory loss, and many more. With such a large number of symptoms, it’s no wonder Chronic Lyme can often go undiagnosed, or even more commonly, misdiagnosed as other diseases. To help better understand the difficulty of differentiating Lyme disease from other diseases we have included a chart from a recent published study in the Medical Microbiology publication which shows the similarity of symptoms between Lyme disease and other commonly misdiagnosed diseases.
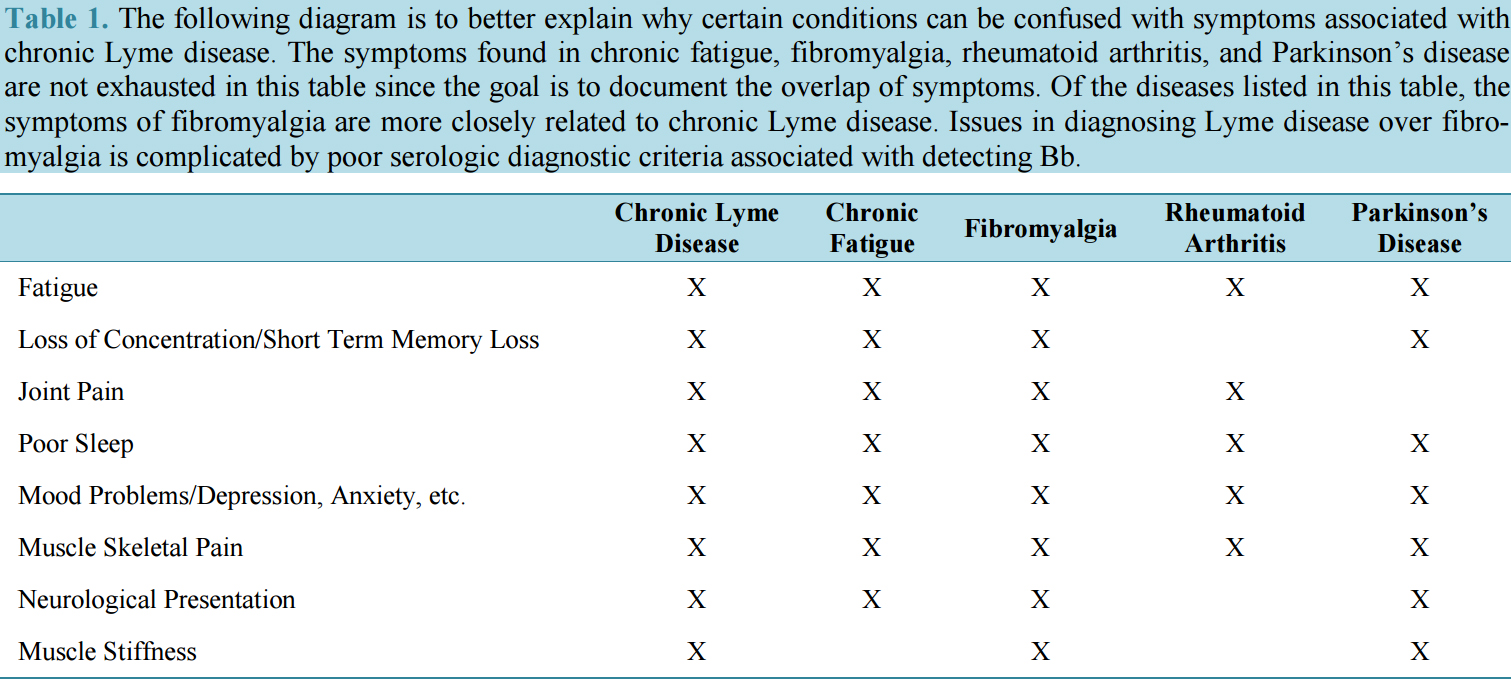
The previous diagram is just a small sample of the many symptoms associated with Lyme disease, but the similarities between Lyme and other common diseases can be easily seen.
How Lyme Disease is Transmitted
Lyme disease is most commonly transmitted by the bite of a blacklegged tick. This type of tick is most common in the north-eastern areas of the United States, but it is important to know that Lyme disease has spread to 49 states (excluding Hawaii) and is becoming an international epidemic. Blacklegged ticks are the primary transmission method for Lyme disease but the ticks also carry other tick-borne infections. These infections decrease host immunity and allow secondary co-infections known as opportunistic infections to wreak havoc on the patient’s body when Lyme disease is present. These tick-borne and secondary co-infections can most commonly include Babesia, Ehrlichia, Cytomegalovirus, Epstein-Barr, Bartonella, and HHV-6 among others.
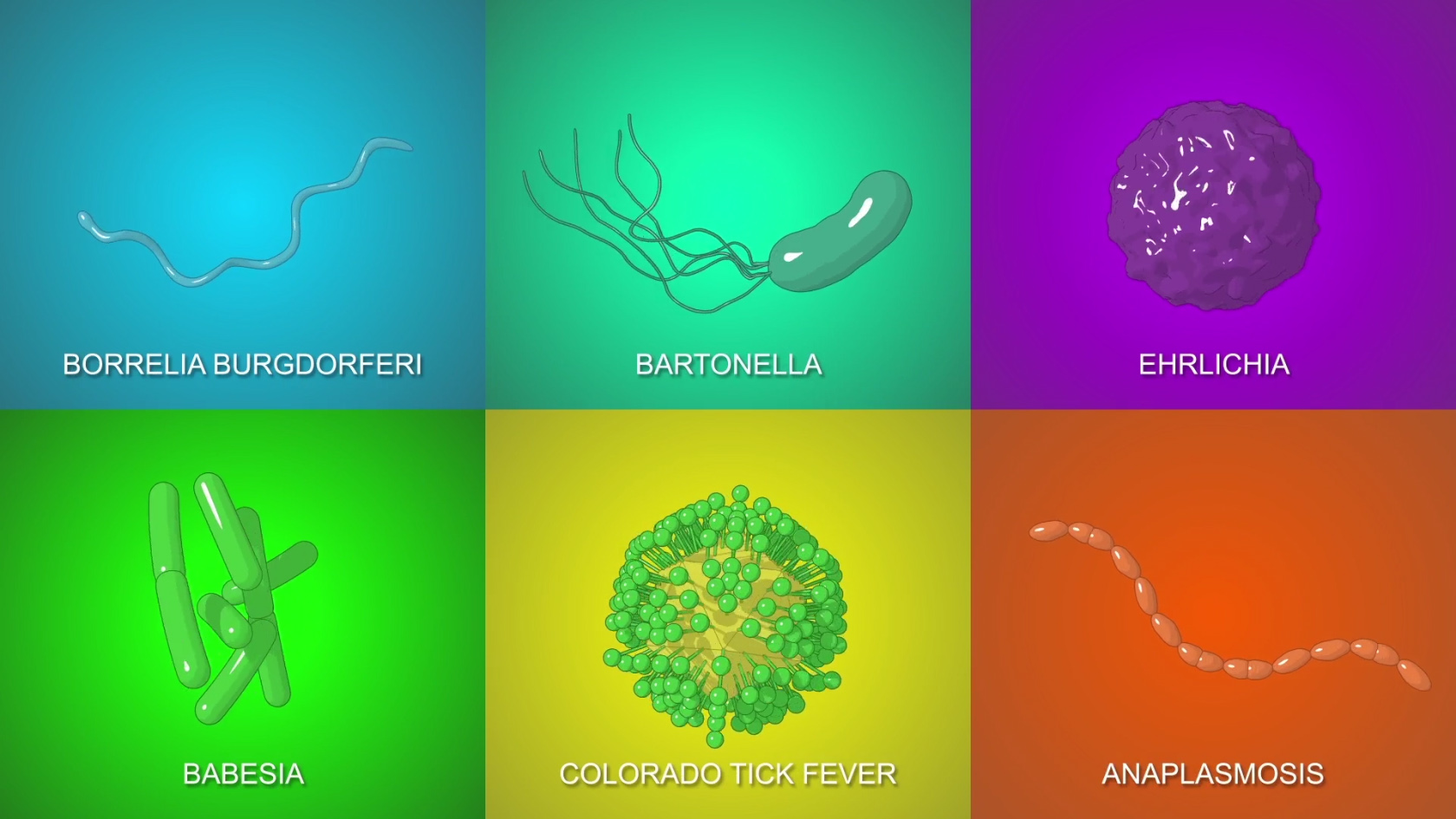
Coinfections
Lyme Disease Diagnosis Difficulties
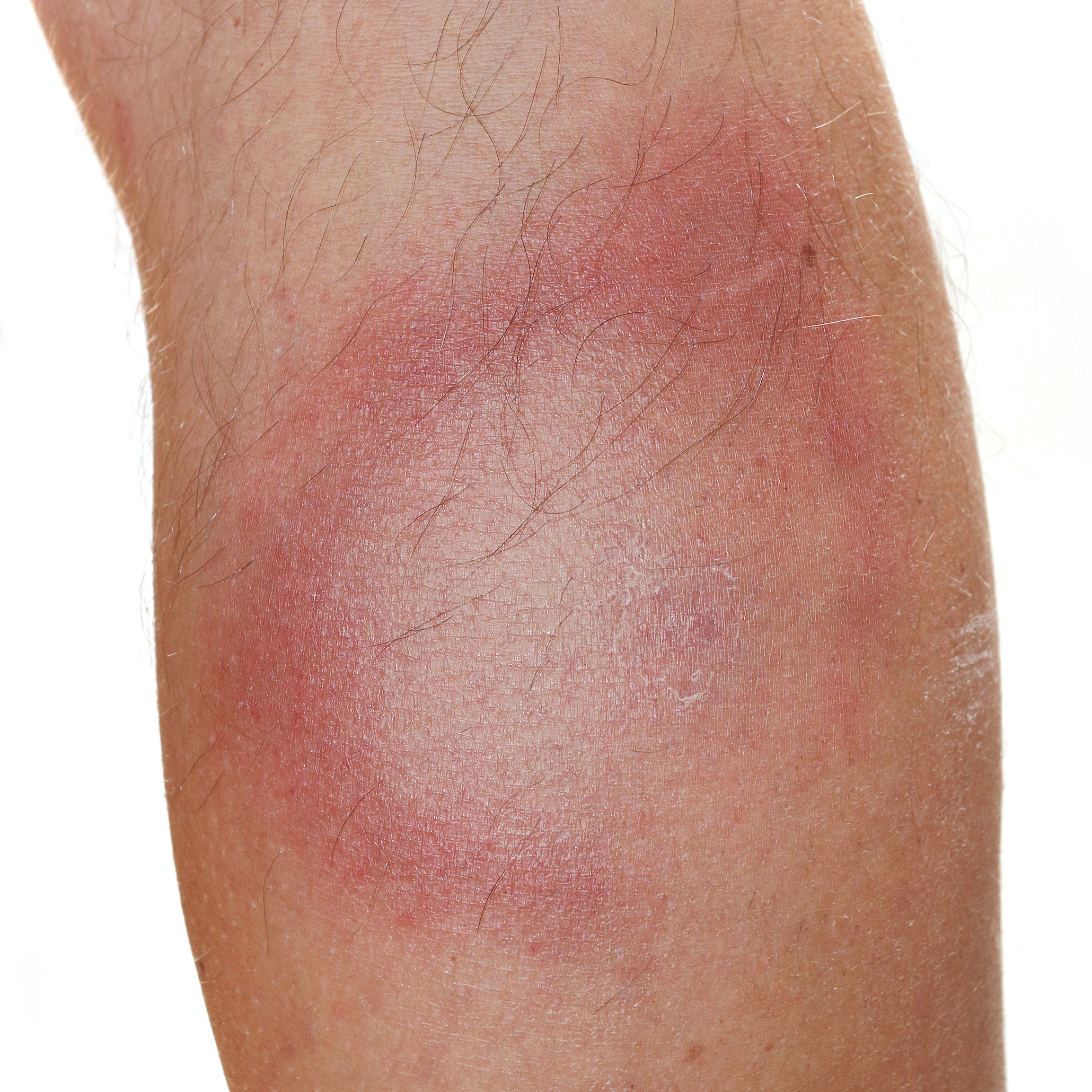
When it comes to diagnosing Lyme there is only one truly accurate tell-tale sign and that is the appearance of a bullseye rash.
While this symptom is a dead-giveaway, not all Lyme disease patients develop the rash, in fact about 50% of Lyme disease sufferers never develop, nor have any recollection of a rash ever being present.
Lyme disease is caused by the bacteria Borrelia Burgdorferi. Borrelia is a spirochete, a cousin of the syphilis family of diseases. The bacteria’s unique corkscrew like shape gives it special properties which can help it evade the body’s immune system and often times antibiotic treatments.
Lyme Disease Treatment
For the treatment of Lyme disease, early detection is key. If the disease is detected early enough a course of antibiotics can usually take care of the disease. It is when the disease has gone undiagnosed or becomes multi-drug resistant that the symptoms of Lyme persist, become chronic and exacerbated and incredibly difficult to treat.
When Lyme disease has gone undiagnosed and/or is not properly treated early enough the condition becomes what is known clinically as Chronic Lyme Disease Complex to Lyme literate physicians. This complex of Lyme disease and its many co-infections can be very difficult to treat but it is important to seek out proper diagnosis before pursuing treatment.
Lyme Disease Testing
The most common Lyme disease tests are the Western Blot and Elisa test. While these standardized tests are considered the correct way to diagnose Lyme disease, they can often produce false-negative results. These tests rely on the body’s immune status and the production of antibodies to detect the disease. Because Lyme disease is so evasive often times the immune system isn’t producing these antibodies to allow for proper diagnosis.
This is why patients who suspect they may have Lyme disease need to seek out specialty labs for a more accurate diagnosis. One such specialty lab is IGeneX. IGeneX looks at samples of the patient’s blood under a microscope. This inspection allows them to visualize and identify “bands of” the spirochetes involved with Lyme disease. IGeneX also runs a separate co-infection panel to help diagnose the other infections that can be present with Lyme disease. It is important to mention that this test is only a starting point. There is a number of specialized tests and labs that must be ran to aid in proper and complete diagnosis to create a full medical blue print for Lyme disease and all the co-infections that can be present.
https://www.envita.com/lyme-disease/lyme-disease-and-the-many-symptoms-it-can-present-in-humans
